The dominant thinking in evolution focuses on inheritance between parent and offspring – or ‘vertical gene transfer (VGT)’.
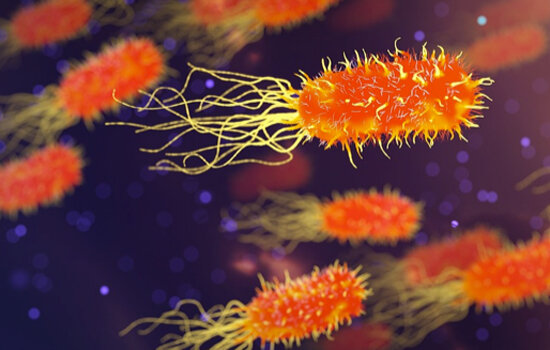
But now scientists are paying more attention to ‘horizontal gene transfer (HGT)’: the transmission of DNA other than from parent to offspring, as this transfer can tell us about the evolution of a number of other organisms such as bacteria. It can also help us to better understand antibiotic resistance.
In a world first, Monash University scientists have discovered that HGT can bend the rules of evolution.
The discovery is outlined in a study published today in PNAS, which was led by ARC Future Fellow Dr. Mike McDonald and Ph.D. candidate Laura Woods, both from the Monash University School of Biological Sciences.
“HGT is very important in microbial evolution, especially for the evolution of antibiotic resistance in human pathogens,” said Dr. McDonald.
Find your dream job in the space industry. Check our Space Job Board »
“Genes for antibiotic resistance in the bacteria that live in hospitals, sewers and farms, are common because there are antibiotics in these places, due to human activities,” he said.
“However, when scientists check environments without antibiotics, for example, forests or estuaries, antibiotic resistance genes can still be detected.”
Dr. McDonald and his team of researchers conducted an evolution experiment to study how the genes that cause antibiotic resistance spread in the environment.
They tested antibiotic-sensitive bacteria in growth media without antibiotics. But they allowed this bacteria to receive HGT from other antibiotic-resistant bacteria.
“We used whole genome sequencing to confirm whether the genes for antibiotic resistance were spreading in the populations, even without selection,” Dr. McDonald said.
“Later we challenged our evolved populations with high concentrations of antibiotic.
“We found that the populations that had received HGT could survive treatment by antibiotic, but the control populations that had not received HGT did not survive.”
The researchers found that antibiotic resistance genes can spread into populations that are not experiencing selection with antibiotic, and that, even though these genes were at low levels, they prepared the population for future challenges with antibiotic.
“This could explain why antibiotic resistance evolves so quickly in hospitals,” Dr. McDonald said.
“Our study shows for the first time how antibiotic resistance genes can stay in a population, even when there is not antibiotic selection pressure,” he said.
“This could also explain why patients still have antibiotic resistant bacteria long after they have finished treatment with antibiotic and why bacteria quickly evolve resistance even when they have not been exposed to antibiotic before.”
Dr. McDonald said the study was important because showed how HGT can bend the rules of evolution.
It was previously thought that the only genes that could spread through a population were those that caused a benefit ‘right now’ (in the environment that the population is experiencing at that point in time).
This is because natural selection should push low fitness, deleterious genes out of the population.
“But our work shows that if HGT can transfer enough of the gene into the population, it can provide a force that pushes back against natural selection, and allows genes that do not confer a benefit to spread in the population,” Dr. McDonald said.
Provided by: Monash University
More information: Laura C. Woods et al. Horizontal gene transfer potentiates adaptation by reducing selective constraints on the spread of genetic variation. PNAS (2020). www.pnas.org/cgi/doi/10.1073/pnas.2005331117
Image: Scientists checked environments without antibiotics, for example, forests or estuaries, and found antibiotic resistance genes could still be detected.
Credit: Monash University