EPFL researchers have developed a device that can zoom in on previously invisible cells at the back of the eye. The technology could be extremely useful for ophthalmologists, in particular for detecting age-related macular degeneration early and assessing new treatment options.
There is renewed hope for people with eyesight problems such as age-related macular degeneration, or AMD. This medical condition affects 26% of people over the age of 60 in Europe and is one of the main causes of blindness in developed countries. A new device developed by researchers at the Laboratory of Applied Photonics Devices (LAPD), which is headed by Professor Christophe Moser, will make it possible to diagnose the condition early, setting the stage for better treatment. The device is the subject of an article published in Nature Photonics this week.
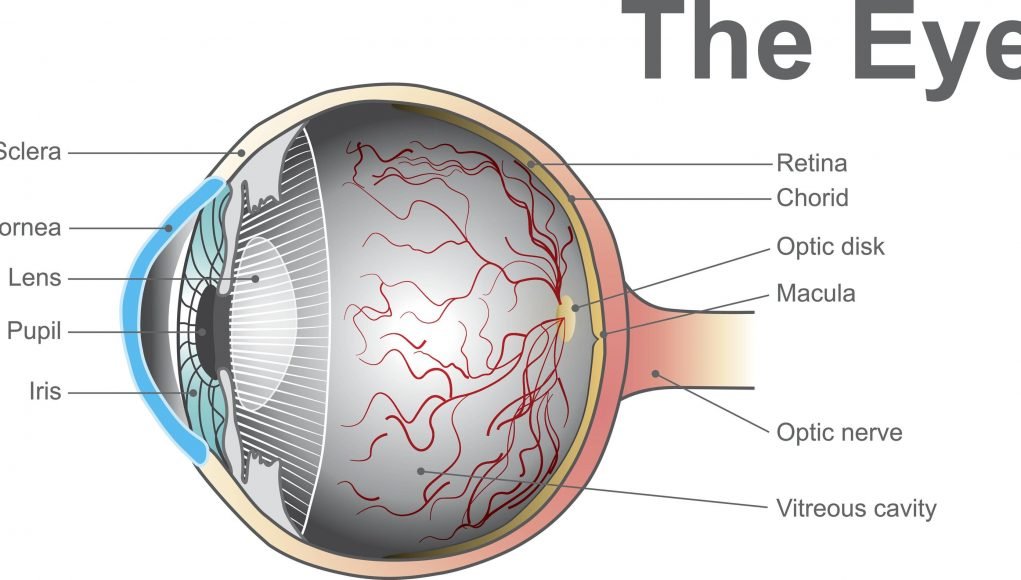
The retina is a complex tissue made up of several layers of cells. It includes the macula, a light-sensitive area at the back of the eye. The macula is responsible for our high-acuity vision, so it is what allows us to read, recognize faces and pick out details. We still don’t really know why, but the macula degenerates over time. This can cause blurry patches or wavy lines to appear in our central field of vision, with peripheral areas remaining intact.
AMD is usually only detected once these symptoms have appeared, which means that the condition is already at an advanced stage. There is not yet a cure, but the effects can be slowed. If AMD could be diagnosed earlier, it could be treated more effectively. That’s where the technology developed by EPFL researchers comes in. It uses a sophisticated imaging system to view the macula cell layers—the first ones affected by AMD—in real time. Routine procedures up to now could not detect these cells, making it impossible to monitor them.
“These cells are where most common retinal conditions originate. Being able to see them will help us to gain insight into how these conditions evolve so that we can detect them earlier and treat them more effectively,” says Francine Behar-Cohen, a professor of ophthalmology at the Hôpital Cochin and a research director at the Centre de Recherche des Cordeliers, in Paris.
Find your dream job in the space industry. Check our Space Job Board »
“Unlike conventional devices, which send light to the center of the pupil, ours looks at the retina through the sclera, which is the white of our eyes,” explains Mathieu Künzi, a researcher at the LAPD and co-author of the study. “This means we get to see the back of the eye from a different, diagonal angle,” adds Timothé Laforest, another LAPD researcher and co-author. “That prevents some of the interference that can come from reflected light and gives us a better view of the cell layers.” The two young researchers have created a startup—EarlySight—to develop and promote this technology in the medical world.
Tests conducted on around a dozen healthy people have shown that the device is reliable. It is ten times more accurate in observing the back of the eye than conventional methods, and it can show the different stages that those cells go through, particularly during the aging process. More in-depth studies on around 50 patients, some of whom already have AMD or other conditions, will be conducted over the coming months.
Provided by: Ecole Polytechnique Federale de Lausanne
More information: Timothé Laforest et al. Transscleral optical phase imaging of the human retina. Nature Photonics (2020). DOI: 10.1038/s41566-020-0608-y
Image Credit: Ecole Polytechnique Federale de Lausanne